It’s fairly common knowledge that health conditions don’t occur inside an isolated bubble. There’s a variety of factors that can either decrease or increase your chances of developing a condition. That’s one of the reasons why your doctor’s office likes to ask about things like diet, exercise, and your family health history.
Today we’re going to hone in on one specific factor — genetics. Keep reading to learn more about how your genetics can impact your vascular health.
Vascular Health
The vascular system (otherwise known as the circulatory system) is comprised of small vessels that carry blood and lymph throughout the body. Your arteries and veins, for example, are a part of your vascular system.
Although seemingly small, all of these small vessels have a huge role to play in your overall body’s health. Your arteries carry oxygen-rich blood from your heart, distributing it across your body. Veins, on the other hand, carry the deoxygenated blood back up to your heart for reoxygenation. Combined, these vessels make up your vascular system.
Something to keep in mind, however, is that this system does need to be cared for. Vascular diseases can affect these daily functions leading to things like high blood pressure, strokes, chest pain, and more.
Genetics And Your Vascular Health
Yes, your genetics do play a large role in the types of health conditions that you are susceptible to. This includes vascular diseases. After all, genetics are the blueprint for how your body is built. For example, everything from the way your veins are made down to how likely you are to have hypertension can be affected by genes.
Having said that, do keep in mind that genetics do not account for all of the risk factors. Your lifestyle (activity level, foods you eat, smoking, alcohol intake) have a large impact as well. Tell your doctor if you have a family history of vascular diseases, and ask for some lifestyle recommendations. They may recommend things like physical activity or a healthier diet.
What Is Vascular Disease?
Vascular disease is an umbrella term used to describe medical conditions that affect your vascular system. This can include anything from blood disorders to diseases of the arteries or veins. Many of these conditions are fairly serious and can even be life-threatening. That’s why it’s so important to learn a little bit more about the various types of vascular diseases and how to reduce your risk of developing one. Vascular disease is particularly common in the US, and the leading cause of death according to the CDC.
Here are two common examples of vascular diseases:
Peripheral Arterial Disease (PAD)
Peripheral arterial disease occurs when arteries begin to narrow, reducing blood flow to arms or legs. This narrowing typically occurs as a result of fatty deposit build-ups. A family history of PAD, obesity, high blood pressure, and high cholesterol are common risk factors for this condition.
Deep Vein Thrombosis (DVT)
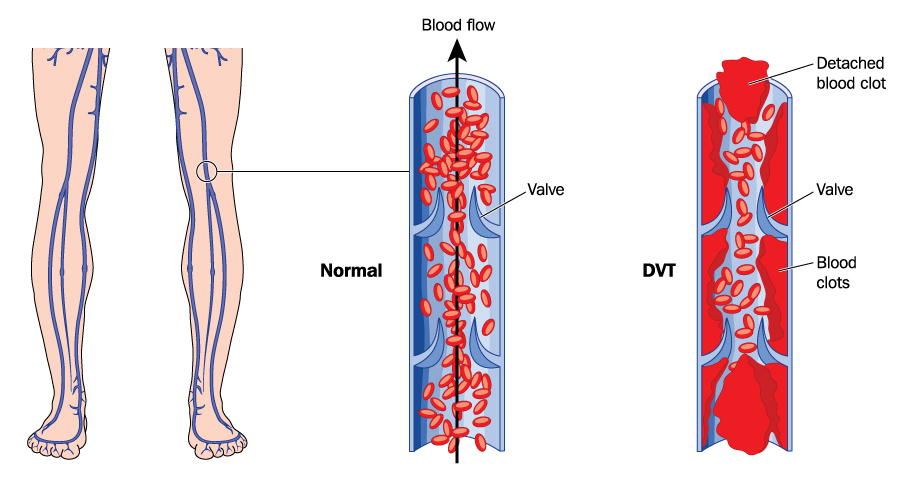
DVT is a condition during which a blood clot forms in a deep vein. These blood clots most often form in the legs, although on rare occasions, they can occur elsewhere in the body. Deep vein thrombosis can cause leg pain or swelling but can also be symptomless.
On rare occasions, a blood clot can break loose, traveling to other parts of the body. This can be fairly dangerous since the blood clot could potentially break loose and travel to the lungs and get stuck, causing a pulmonary embolism.
Chronic Venous Insufficiency (CVI)
Another common term you may want to know a little bit about is Chronic Venous Insufficiency (CVI). You may have already seen this term used in our other articles, however, since it’s closely related to varicose and spider veins.
Generally speaking, CVI is when your veins are no longer able to move blood flow along as well as they should. This is typically due to damaged vein valves. As blood stagnates, it can even pool within the vein, causing an increase in the pressure against the walls of the vein. This can often result in what we refer to as varicose or spider veins.
Although there are a variety of factors that can increase your risk of developing CVI, a family history of the disease is one of them.
Varicose Veins
As we mentioned above, varicose veins occur when blood stagnates or flows backward. The blood pools and begins straining against the walls of the vein. The result is an enlarged, twisted vein that is bluish or purplish in appearance.
Are Varicose Veins Genetic?
Unfortunately, genetics does play a large factor in the development of varicose veins. Many patients that develop varicose veins have a family history of the condition. Age and gender can play large roles as well since many people develop varicose veins as they get older, and women are particularly prone to this.
Having said that, it’s important to note that there are some factors that are more controllable. For example, excess weight and standing or sitting in one position for long periods of time have both been linked to varicose veins as well. The best thing you can do is stay active and maintain a healthy weight in order to minimize your risk as much as you can.
Spider Veins
Spider veins are generally a similar condition to varicose veins, just to a lesser extent. Unlike varicose veins, spider veins are small and web-like in appearance, and can typically be seen near the surface of the skin.
Are Spider Veins Genetic?
Similarly to varicose veins, genetics can affect your risk of developing spider veins as well. Fortunately, there are some great medical treatment options for spider and varicose veins. Talk to one of our vein specialists today to learn more.
What Can You Do?

Now that we’ve talked a little bit about the role of genetics in your vascular health, let’s talk about lifestyle. Your family history and genetics may not be something that you can change, but there are still plenty of steps you can take to decrease your chances of developing a vascular disease by at least a little bit.
The first thing that you should do is make sure that you’re keeping up with your doctor’s visits. Always attend your annual check-ups and have a primary care provider. Your doctor can do things like run labs, take your heart rate, and address anything that seems concerning. Also, don’t forget to let your primary care provider know about any family history of vascular disease. If you happen to be experiencing any unusual symptoms, make sure to mention those as well.
In the meantime, try to take a look at your lifestyle and see if you can make any changes that might benefit your health. For example, eating a nutritious diet with few empty calories is a good place to start. Next, ask yourself if you get enough exercise on a weekly basis. If need be, you can always start with small goals; for example, try to hit at least 10,000 steps per day. A smartwatch or fitness app can help you keep track of your activity.
Although there is no single solution or 100% certain way to prevent all vascular diseases, you can lower the risk by leading a healthier lifestyle.
Flint Vein Solutions
Tired of pesky varicose and spider veins? That’s what we’re here for. VeinSolutions™ offers effective, minimally invasive treatment options for a variety of venous concerns. Sclerotherapy, venous ablation, and microphlebectomy are just a few of the vein procedures that our clinic offers.
Excellent medical care isn’t the only thing that we offer here, though. First and foremost, we offer empathy and compassion. We know that taking that first step to healthier veins can be difficult, so we do everything we can to make it a little easier on our patients. That’s why our patients love us.
Last but not least, we don’t want to forget to mention that we offer FREE vein screenings here at VeinSolutions™. This means that you have all the information you need before making a decision regarding your veins. Don’t hesitate to book your first appointment with us today. Our office can be reached via our online contact form or at 810-232-3363.



